Our review of new research into vitamin B12
Vegan Society of Canada News
May 16th 2020
In the last few years, there has been interesting new research shedding light on the contentious issues surrounding vitamin B12. In light of this, we are updating our recommendations and remind everyone who self-identifies as vegans to supplement and monitor their B12 levels.
One recent study observed a relation between high vitamin B12 levels with higher rates of mortality and cancers. This study published early this year came to the following conclusion:
In this population-based cohort study including 5571 adults, higher plasma concentrations of vitamin B12 were associated with a 25% increased adjusted risk of all-cause mortality per 1-SD increase.
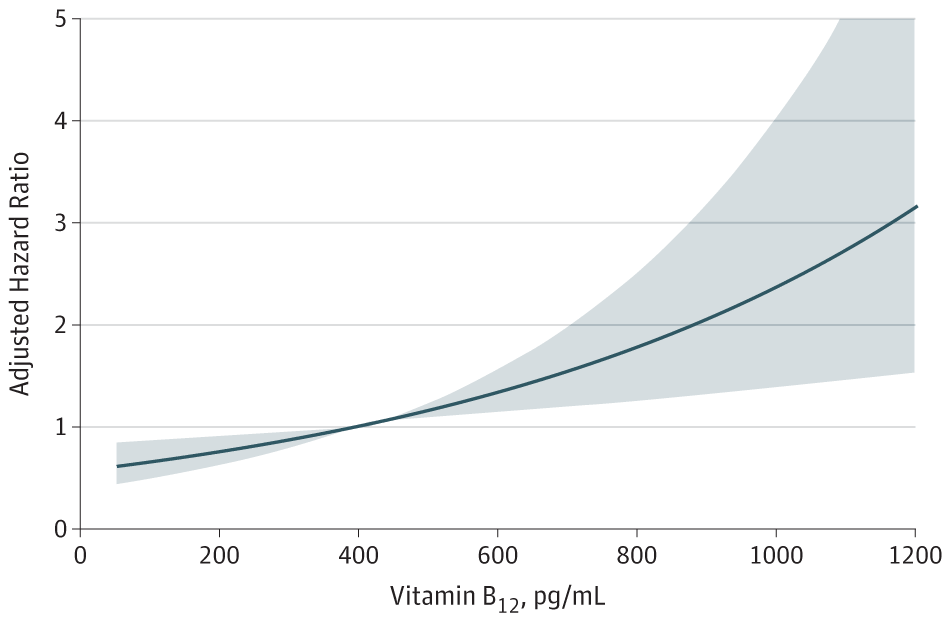
After reviewing the study, we believe that the results seen here are what many other studies have reported: An increase in consumption of animal products results in a higher mortality rate. The authors also acknowledge this, however, their data did not adjust for this:
As the only dietary source of vitamin B12 are animal products, it is possible that the present association could also be explained by the already reported association of higher animal protein intake with all-cause mortality. Unfortunately, the PREVEND cohort does not include data on dietary patterns. Our analyses were conducted after the exclusion of individuals who were prescribed with injectable vitamin B12 supplementation at the baseline measurements, nonetheless the Pharmacy records have no available information about the over-the-counter tablets of vitamin B12, and therefore our results cannot be adjusted for such variables.
Previous studies have demonstrated that vegans do not carefully monitor their B12 levels, which tend to be lower than it should be. In addition, B12 levels in the general population is probably one of the best proxy for the consumption of animal products. As such, it seems logical that this study is once again confirming that a diet high in animal products sees a higher mortality rate. Unfortunately, the researchers involved with this study did not have a vegan control group so its usefulness is limited. While there are other questions and issues with the results, this is by far the most important.
As we have done before, where lifestyle habits may be the actual cause for what is observed, we urge future researchers in the topic of high levels of B12 and mortality rate to use various groups like vegans as a control so we can know if the increase consumption of animal products is the cause of increasingly higher mortality rates seen in this case.
In normal circumstances, we would have waited for future research to come along to confirm or disprove our hypothesis. One of the issues we have is that, until now, there has been no scientific evidence proving that B12 is harmful at high level, and no scientific evidence proving that B12 above a certain level, around 300-400 pmol/l, is beneficial.
However, the problem we were faced with is that even if there is just a 0.0001% chance of a high level of B12 itself causing a higher mortality rate, that would still be more than the 0% benefit we get from a level higher than 400 pmol/l. In addition, while the shape of the curve may be in question, especially in the 300–400 pmol/l range, this question is purely academic for the time being since there was never any benefit to higher levels. Furthermore, this research is not the first to raise potential issues with high levels of B12; there were at least two others, one by Brasky et al. (2017), and one by Fanidi et al. (2018) that raised issues with high B12 and lung cancer, which conflict with the result of this research.
Our position is that it seems probable that the issues are associated with the high consumption of animal products, not B12 itself.
In the last few years, the role of B12 in cardiovascular disease also became clearer. The National Institutes of Health’s latest opinion refers to the American Heart Association statement in 2006
Evidence supports a role for folic acid and vitamin B12 supplements in lowering homocysteine levels, but results from several large prospective studies have not shown that these supplements decrease the risk of cardiovascular disease.
The American Heart Association has concluded that the available evidence is inadequate to support a role for B vitamins in reducing cardiovascular risk.
However, a recent investigation shows that the conflicting results from those studies came from cyanocobalamin’s effect on patients with impaired renal function, hiding the benefits of vitamin B on patients with good renal function.
In 2017, with Yi and Hankey, we performed a meta-analysis of the trials stratified by dose of cyanocobalamin and by renal function. In addition, we analyzed patient-level data from the VISP trial and the VITAPOPS trial. What emerged was that harm from high-dose cyanocobalamin among study participants obscured the benefit of B vitamins among study participants with good renal function.
In addition, there is also scientific evidence building that for certain people, e.g. people with diabetic nephropathy, the use of cyanocobalamin over other forms of B12 precipitates decline in renal function. Therefore, to prevent any potential issues, since early stages of diabetic nephropathy tend to be asymptomatic, we will echo the recommendation of the researchers and recommend B12 in methylcobalamin form for oral supplementation.
In patients with diabetic nephropathy, folate/B6 and cyanocobalamin 1,000 μg daily accelerated the decline of renal function and doubled cardiovascular events. Patients with renal failure have high cyanide levels.
Therefore, folate alone is not the optimal way to lower tHcy: the use of folate (and possibly B6) with methylcobalamin or oxocobalamin should be considered.
It’s important to note that there is no evidence for healthy adults that the cyanide content in cyanocobalamin is a problem. There is already a small amount of cyanide in much of the food we eat today, and for a healthy adult this has not proven to be a problem. As a reference, the minimal risk level established by the Agency for Toxic Substances and Disease Registry for cyanide is 50 mcg/kg per day, and the European Food Safety Authority is 20 mcg/kg per day, and a 1000mcg vitamin B12 contains 20 mcg of cyanide. However, we recently discovered that for adolescents and particularly children these thresholds can be breached with everyday food intake. In research published in 2019, the European Food Safety Authority stated:
At the 95th percentile, the ARfD was exceeded up to about 2.5‐fold in some surveys for children and adolescent age groups. The main contributors to exposures were biscuits, juice or nectar and pastries and cakes that could potentially contain CNGs. Taking into account the conservatism in the exposure assessment and in derivation of the ARfD, it is unlikely that this estimated exceedance would result in adverse effects. The limited data from animal and human studies do not allow the derivation of a chronic health‐based guidance value (HBGV) for cyanide, and thus, chronic risks could not be assessed.
Since cyanide is a poison, and while thought to be safe at levels below 20 mcg/kg of body weight, it nevertheless provides no health benefit—similar to pesticides being present in much of the foods we eat and thought to be safe below certain levels. In addition, while it may be difficult to avoid cyanide in foods we consume every day, it is easily avoidable in our B12 supplements, albeit at a higher price.
Clarity was also provided around vitamin B12 and its impact on various medications, like those to treat heartburn and diabetes, which may affect the absorption of vitamin B12. There is still a lot that we do not know, but we support the advice in the research published by Miller (2018):
This suggests that prudent clinical practice would be to assess vitamin B-12 status when starting PPIs, H2RAs, or metformin prescriptions and monitoring it on a regular basis (e.g., every few months).
As well as the research from Nehra (2018) which states:
However, as this story evolves, our current practice is to check creatinine levels yearly, complete blood cell counts every other year, and vitamin B12 levels every 5 years in patients receiving long-term PPI therapy.
Therefore, after evaluating all of this new research, we have revised our B12 recommendation to the following:
- B12 lower bound remains the same, with symptoms of deficiency having been observed in some cases as high as 249 pmol/l.
- B12 optimal remains the same, thought to be around 300-400 pmol/l.
- As a precaution, a B12 upper bound at 400 pmol/l.
- Methylcobalamin as a general recommendation for oral supplements, with Cyanocobalamin as an option for healthy adults.
What B12 intake level will be needed to achieve these levels will depend on each individual and various factors, for example, age and medications. As our intrinsic factors diminish with age, we recommend doing regular tests. This latest paper published in 2019 discusses in detail the various aspects of B12 deficiency and suggests a novel mathematical formula to address all the pitfalls with individual B12 measurements like blood serum, MMA, HoloTC and homocysteine.
A more mathematical approach toward establishing vitamin B12 deficiency was proposed by Fedosov et al, who calculated a single combined indicator of vitamin B12 status in which levels of total serum vitamin B12, holoTC, MMA, and homocysteine are taken into account. This is an elegant approach to making a proper diagnosis, but its validation in the context of both functional vitamin B12 deficiency and systematically evaluated response to vitamin B12 supplementation therapy is required.
There are multiple testing regimes and intake levels suggested by various people and/or organizations. Many of them are around those levels:
- 10-50 mcg once per day
- 4.5 mcg 3 times per day
- 2000 mcg once a week
- 1000 mcg per day over 65 years old
In an ideal world, we would have vitamin and mineral intake levels tailored to each individual. Unfortunately, this is far from being efficient at this time, so the best alternative we have is to take a large sample of the population and try various intake levels to find one that minimizes deficiencies and toxicity while maximizing those around the optimum level. As far as we know, this process has never been done on a vegan population, and what we are left with is inadequate overall population recommendations.
Therefore for people who have never had their B12 levels tested, we suggest getting tested first as this will determine if you are currently deficient and if your current regimen is adequate. It’s probable that it will not be sufficient, in which case a decision will have to be made whether one tries to attain the optimal level with fortified foods, for example by using a combination of fortified nutritional yeast and plant milk, or with supplements. After that, it’s simply a matter of fine tuning with testing until the optimum level is reached and then maintain those levels of supplementation.
Additionally, we should keep an eye on our levels as we age and increase supplement intake as appropriate to maintain optimum levels. As it is recommended to start testing lipid profiles every 5 years starting at around 35–50 years of age—and pernicious anemia is rare below 50 years old, while stores of B12 can last 3–5 years—it seems a good idea to add B12 tests to regular blood tests and adjust as necessary.
Please keep in mind that since the risk is much more on the downside, unless someone is above 400 pmol/l and willing to not only change their intake level but also retest to ensure their new regimen produces optimum levels, we would advise not to change anything at this time.
Please discuss with your health-care professional to take into account your specific situation.